Have you ever found yourself breathless after climbing a flight of stairs, or feeling unusually fatigued after a simple walk? These seemingly mundane experiences could be more than just signs of being out of shape. They might be early warning signs of Pulmonary Arterial Hypertension (PAH). Understanding this condition and recognizing its symptoms early can make a significant difference in your health journey. In this post I will explain PAH deeper and also describe my personal experiences and how I got to the doctors.
What is Pulmonary Arterial Hypertension?
Pulmonary Arterial Hypertension (PAH) is a rare but serious condition characterized by high blood pressure in the arteries that supply the lungs. Unlike regular hypertension, which affects the entire circulatory system, PAH specifically impacts the pulmonary arteries, leading to various complications if left untreated. Early detection is crucial to managing this condition effectively.

As you can see above, a healthy artery can have blood flowing as it should, however when the arteries become narrowed it makes it harder for the blood to flow through them causing in high pressure in the arteries – which is PAH.
The Subtle Symptoms of PAH
One of the challenges in diagnosing PAH is that its early symptoms can be quite subtle and are often mistaken for less serious conditions. Here are some key signs to watch for:
- Shortness of Breath: This is the most common symptom of PAH. Initially, you may notice it during physical activity, but as the condition progresses, even everyday activities can leave you breathless.
- Fatigue: Feeling unusually tired or drained of energy, even after a good night’s sleep, can be an early indicator of PAH.
- Chest Pain: Discomfort or pain in the chest, especially during physical exertion, can be a sign that your heart is working harder than usual to pump blood through narrowed pulmonary arteries.
- Dizziness or Fainting: Experiencing lightheadedness or episodes of fainting can occur as PAH progresses, due to the strain on your heart and reduced oxygen levels in your blood.
- Swelling: Edema, or swelling in the ankles, legs, or abdomen, can be a sign of advanced PAH as the heart struggles to pump blood efficiently.
Causes of Pulmonary Arterial Hypertension (PAH)
Pulmonary Arterial Hypertension (PAH) can be caused by various factors, and understanding these can help in both diagnosing and managing the condition. The causes of PAH are categorized into different groups based on their origins:
- Idiopathic PAH (IPAH):
Unknown Cause: Idiopathic PAH occurs without any identifiable cause. It is considered primary and often affects younger adults. Genetic mutations may play a role, but the exact cause remains unknown. - Heritable PAH:
Genetic Factors: This form of PAH is passed down through families. Mutations in certain genes, such as BMPR2, can increase the risk of developing PAH. - Drug- and Toxin-Induced PAH:
Medications and Substances: Certain medications, like appetite suppressants (e.g., fenfluramine and dexfenfluramine), and illicit drugs (e.g., methamphetamines and cocaine) can lead to the development of PAH. - PAH Associated with Other Conditions:
- Connective Tissue Disorders: Diseases like scleroderma, lupus, and rheumatoid arthritis can cause PAH.
- Congenital Heart Disease: Defects present at birth, such as Atrial Septal Defect (ASD) or Ventricular Septal Defect (VSD), can lead to PAH.
- Liver Disease: Conditions like portal hypertension can contribute to the development of PAH.
- HIV Infection: People with HIV are at a higher risk of developing PAH.
- Chronic Hemolytic Anemia: Disorders like sickle cell anemia can lead to PAH.
- Schistosomiasis: This parasitic infection can cause PAH, especially in endemic areas.
- Persistent Pulmonary Hypertension of the Newborn (PPHN):
Newborns: This rare form affects newborns and is characterized by high blood pressure in the lungs’ arteries shortly after birth, often due to complications during delivery or other perinatal factors. - Secondary Causes:
- Left Heart Disease: Conditions like left-sided heart failure or mitral valve disease can cause secondary pulmonary hypertension.
- Chronic Lung Diseases: Diseases like chronic obstructive pulmonary disease (COPD) and interstitial lung disease can lead to pulmonary hypertension.
Understanding the underlying cause of PAH is crucial for proper diagnosis and treatment. If you experience symptoms like shortness of breath, fatigue, chest pain, dizziness, or swelling, it’s essential to consult a healthcare provider for a thorough evaluation.
The Importance of Listening to Your Body
Self-diagnosis can be a tricky and often risky, especially with a condition as serious as PAH. However, being aware of these symptoms and how they interconnect can prompt you to seek medical advice sooner rather than later. Here’s how you can become more in tune with your body’s signals:
- Keep a Symptom Diary: Track your symptoms, noting when they occur and their severity. This information can be invaluable to your healthcare provider.
- Monitor Physical Activity: Pay attention to how your body responds to exercise and everyday activities. If you notice a decline in your ability to perform tasks that were previously easy, it’s worth discussing with a doctor.
- Stay Informed: Educate yourself about PAH and its symptoms. The more you know, the better equipped you’ll be to recognize potential warning signs.
Seeking Professional Help
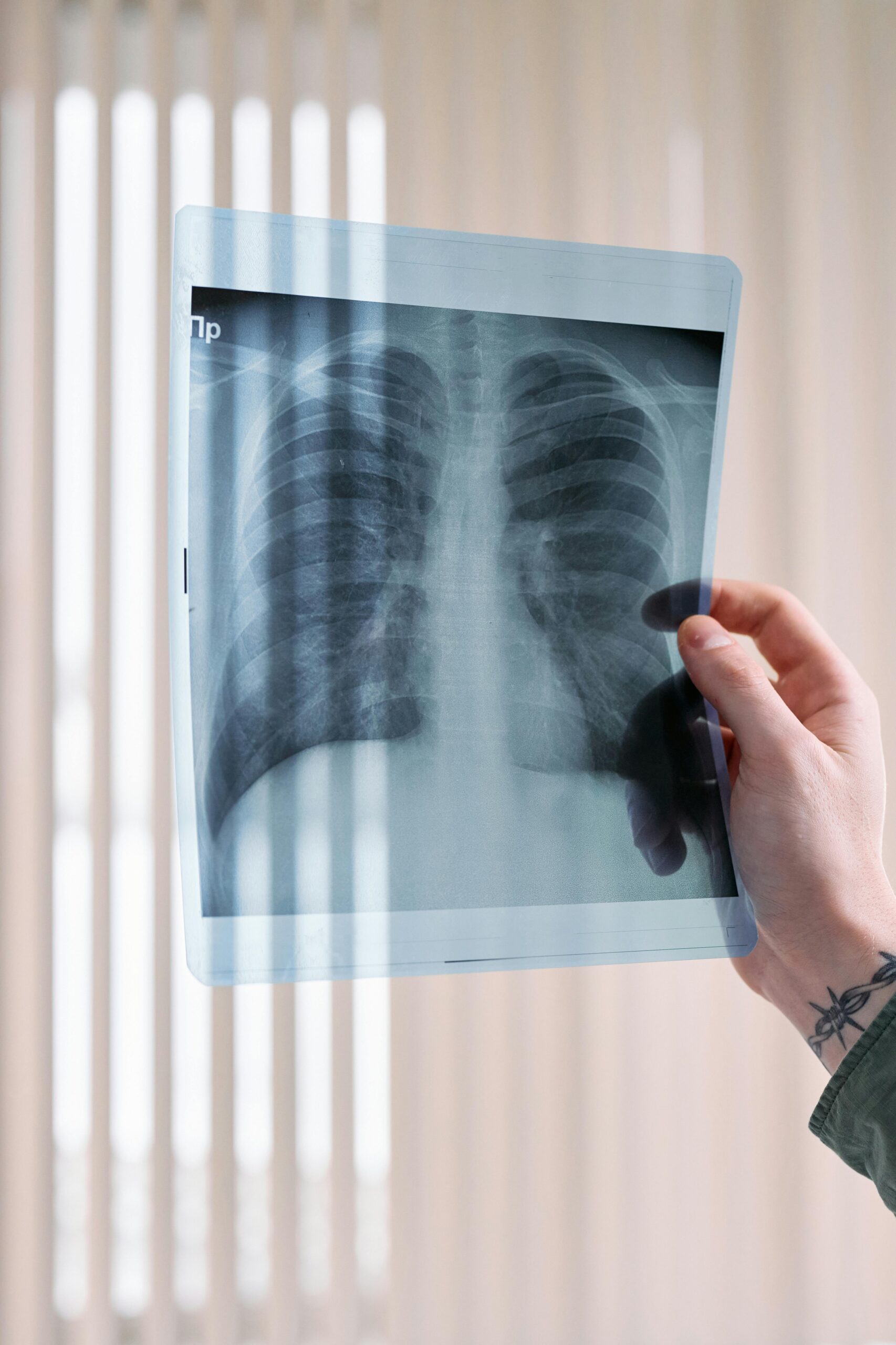
If you suspect you might have PAH, it’s crucial to consult with a healthcare professional. Diagnosing PAH typically involves several tests, including echocardiograms, chest X-rays, and right heart catheterization. These tests can confirm whether you have PAH and determine its severity.
Personal Experiences
About a year before my diagnosis, I began experiencing severe shortness of breath. Walking on flat ground for just three minutes left me puffed out. Initially, I attributed it to a lack of exercise and weight gain, so I lost around 8 kg and started exercising daily. However, the improvement was minimal, and I still found myself easily out of breath.
A close friend noticed my breathlessness and recommended I see a GP. The doctor conducted a series of tests, starting with an ECG. The results showed irregular patterns, which the doctor explained were similar to those seen in heart attack patients. They requested a chest X-ray, but I had to wait 10 months due to my young age and lack of other health issues, which likely made me a lower priority.
When the X-ray results finally came in, they revealed that my arteries were not clear; they appeared cloudy. This led to a request for an echocardiogram, which ultimately uncovered that I had both Atrial Septal Defect (ASD) and Pulmonary Arterial Hypertension (PAH).
Conclusion
While self-diagnosis has its limitations, being proactive about your health and recognizing the early symptoms of PAH can lead to timely medical intervention and better outcomes. What I regret is that I didn’t go to the GP earlier and not following up with the doctors for my chest x-ray. During the 10 months I felt my symptoms worsened. Please remember, your health is your most valuable asset. Don’t ignore the signs your body is giving you. Stay informed, stay vigilant, and take action if you suspect something isn’t quite right. Your journey to better health starts with awareness. If your body doesn’t feel normal and you experience symptoms like those described above or find yourself unusually breathless, go see a doctor. Even if it’s not PAH, getting checked out will be definitely worth it.